DEFINITION
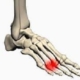
The Achilles tendon is the terminal tendon of the Sural Triceps (calf muscle), it is richly innervated, but poorly vascularized.
Achilles tendonitis or Achilles tendonitis therefore manifests itself by inflammation of the Sural Triceps at the level of its insertion on the calcaneus (heel bone).
Achilles tendonitis is usually mechanical (sometimes inflammatory).
It is a common condition in athletes.
The clinical diagnosis of tendonitis is characterized by pain on palpation, pain in stretching, and pain in upset contraction.
Note that the term tendonitis is gradually replaced by the term tendinopathy, which more generally designates a condition of the tendons.
CAUSES
Mechanical Achilles tendinitis can occur during violent trauma or during intense physical activity without preparation with a shoe that is unsuitable for the terrain.
Very often, it is consecutive to a retraction of the Triceps Sural called “Achilles court”.
When walking and running, the Achilles tendon will work excessively and be stretched too much. By dint of being subjected to constraints and micro trauma, he will suffer and eventually become inflamed.
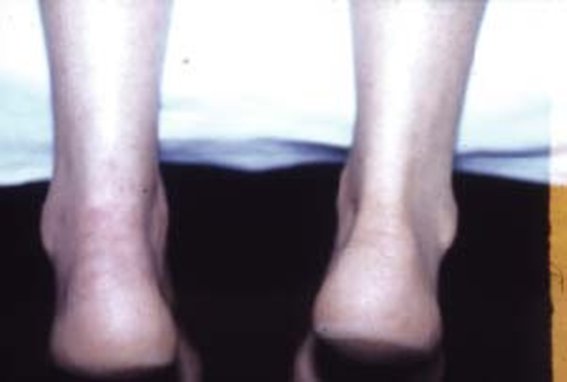
Static disorders such as a valgus or varus hindfoot, a hollow foot (verticalization of the calcaneus) or a Haglund (posterior tuberosity of the calcaneus which will modify the path of the Achilles tendon and compress it) are also responsible for Achilles tendinopathies .
When Achilles tendonitis is expressed bilaterally, we must think of more unusual etiologies such as certain classes of antibiotics (quinolones), a dental infection, an excess of uric acid or the complication of rheumatoid arthritis.
SOLE TREATMENT
Treatment depends mainly on the etiology.
In the case of Achilles tendonitis of mechanical origin, the basic treatment consists in stopping all activity. If this treatment proves effective, it remains nonetheless restrictive. It seems difficult to ask a patient to consider a rest period of six to eight weeks.
This is where the podiatrist has an important role to play. The use of an orthopedic sole has all its advantages: on the one hand by bringing the points of insertion of the Triceps Sural closer, on the other hand by taking into account the correction of the associated static disorder.
Some specialists will express their reluctance regarding the use of a heel pad, given the hypo-extensibility of the Sural Triceps. However, it must be recognized that in the acute phase, the patient needs to find an emergency solution to walk painlessly.
At the start of treatment, the heel pad may be indicated. This will then have to be rectified as the pathology progresses. The treatment will be all the more effective if it is accompanied by stretching exercises of the Sural Triceps.
The orthopedic sole is a more judicious alternative to the simple heel pad for the following reasons: the possibility of including a heel compensation with the same characteristics as mentioned above, the possibility of including a heel shock absorber which will reduce micro trauma generated by hitting the heel on the ground, and finally the management of the associated static disorder, the correction of a static disorder in varus or valgus also leading to a decrease in overloading of the Achilles tendon.

Apart from the expertise of the podiatrist to assess the necessary corrections to be made to the sole, advice on the use of appropriate footwear is essential.
To conclude, there are other therapeutic aids to treat Achilles tendinitis (physiotherapy, anti-inflammatory drugs, corticosteroid infiltration, shock waves, etc.) that will vary depending on the stage of the disease and the functional repercussions.
All these treatments should in no case obscure the fact that Achilles tendinitis is generally of mechanical origin, mechanical treatment with a well-adapted sole should not be underestimated.
Christophe Lecourt
Podologist at CAP-PODOTHERAPIE (Lancy and Onex GMO)